Sometimes the greatest success comes from a mistake. Or an accident.
In a drug originally developed to treat Type 2 diabetes, scientists discovered during the process that the active ingredient in these drugs could also be used prescriptively to aid weight loss. Boom, an industry estimated to be worth 200 Billion dollars by 2030 was accidentally born.
So what do you need to know about the trend sweeping social media and dominating the headlines? And why does it matter?
Disclaimer: This article is not intended to be medical advice nor is written from the point of view of any expertise. It is only a deep dive from my own curiosity and interpretation of the data. Please do your own research and consultation with a medical professional before approaching trying any drug or supplement.
Many people have heard of the main contenders – Ozempic, Wegovy, and Mounjaro. In my research and analysis, I am focusing less so on the named brands and more so on the themes common to semaglutide or GLP-1 weight-loss drugs. If you want to read about the popular brands and what the difference is between them I suggest you start here and I will link more articles in the reference. The basic active ingredient and the hormonal-mimicking effect is similar in all of the existing brands.
Love and Other Drugs
In the movie “Love and Other Drugs,” starring Jake Gyllenhaal and Anne Hathaway, Jake Gyllenhaal plays a struggling pharmaceutical sales rep whose world completely changed once he stumbled upon selling Viagra. This is a rom-com, so of course the beginning of the movie is about how he’s an incurable but charming Playboy, who meets THE girl, (Anne Hathaway), who learns what true love is when he falls for a woman who has early stages of Parkinson’s.
SPOILER ALERT: If you like ridiculous grand romantic gestures involving chasing a bus on a highway, you want to watch the whole movie!
The “drugs” storyline was a subplot, but I immediately thought of this when I was researching semaglutides. Both ended up being blockbuster drugs – and were originally intended for other purposes. The famous blue pill was originally a failed treatment for angina. After further investigation during clinical trials, there was a side effect that was quite difficult to ignore. And this medical mistake resulted in a 3 billion dollar industry.
This discovery joins a long list of accidental miracle drugs – including penicillin and antidepressants.

Injectable Semaglutide and the Hollywood Factor
The most perplexing question of 2023: How did a diabetes drug that has been around for years suddenly become the most talked-about treatment for weight loss? You cannot miss discussion about them in newspapers, TV shows, and on social media. Transformation videos dominate TikTok and social media, but Hollywood is credited (or blamed) for its popularity. Even Elon Musk has publicly credited his weight loss for Ozempic.
The Hollywood glitz and glamor associated with miracle drugs is still alive today, for a different sexy product. Thin is officially back in, and celebrities are popularizing drugs like Ozempic, Mounjaro and Wegovy. If they don’t openly admit to taking them, then they are rumored to be doing so. As Andy Cohen famously tweeted in his comment on the craze, “Everyone is suddenly showing up 25 pounds lighter.”

What is a “Semaglutide?”
Semaglutide generally refers to a class of medications. Specifically, it is a glucagon-like peptide-1 (GLP-1) receptor agonist originally FDA-approved to treat type 2 diabetes in 2017. GLP-1 is a hormone produced by the GI tract, and GLP-1 receptor agonists work by binding to certain receptors of this hormone in the body, which are located in the pancreas, brain, and GI tract. When working on the pancreatic receptor, the semaglutide decreases blood sugar – hence, its utility for treating Type 2 diabetes. However, during clinical trials, researchers noticed its potential for weight loss as a separate side effect.
Building on this discovery, a leading pharmaceutical company conducted further studies to specifically assess the drug’s effectiveness in managing obesity. The FDA approved a drug with a higher dose of semaglutide to treat obesity in 2021.

How do these drugs make you lose weight?
As discussed, GLP-1 agonists mimic a hormone that signals satiety and reduces appetite, so people eat less and lose weight. While the historic purpose was originally to lower blood sugar in Type 2 diabetes, a side effect of weight loss became apparent in clinical studies. This primarily was the case because the drugs slow digestion and stomach emptying, making you feel fuller faster, so you eat less. There are GLP-1 receptors in the brain and the gut which when stimulated leads to a decrease in appetite and a delay in gastric emptying. The combined effect leads to drastic weight loss in a short amount of time.
There is also a psychological effect associated with a lack of hunger and resulting “food indifference”. In fact, according to a recent New York Times article, patients reported simply losing interest in food altogether, even foods that they used to enjoy eating. Thus, the power of these drugs does not derive from how they metabolize what you eat.
Think of it this way – a traditional McDonald’s Big Mac and small fry order (without the soda!) is roughly 900 calories. If your appetite is stunted and you find yourself losing interest and/or getting full after eating just half the burger and a few fries, this could result in only a 300-350 calorie meal, which is really low. If all 3 of your meals were like this, even if they are “junk” food, you could be looking at eating just over 1000 calories a day. As I have said previously, while all kinds of diets may emphasize the substance of food over calories, there is far more evidence that weight loss is simply an energy equation of calories in, calories out (CICO).

What about exercise?
Often a huge advantage is that with less eating and hunger, exercise becomes less relevant or even appreciated as necessary. Have you ever noticed when you get sick and lose your appetite, even if you lie in bed all day and all night for days you lose weight? That’s because eating so little is up against your basal metabolic rate calorie burn, which when combined with calories burned from digestion and any incidental activity can vastly outnumber the small amount of food that you end up eating from the medication side effects. (if you need a refresher on CICO and the role of exercise, read my article explaining it here).
Why are these drugs so popular?
What perhaps is most surprising about the popularity of these drugs is that it is part of a shift in our culture back to the worship of thinness. Although this culture seemed to have been a relic of the 90s, like neon scrunchies, it has re-emerged and created a demand for solutions that don’t have patience for going to spin class.
There is also impressive scientific evidence that weight loss actually occurs. For example, in a JAMA study of 175 patients with overweight or obesity, the total body weight loss percentages achieved were 5.9% at 3 months and 10.9% at 6 months. A landmark clinical trial published in The New England Journal of Medicine in 2021 found that the drug led to a 15% reduction in body weight, on average. Most of that weight is lost in the first month, meaning that people are losing 10-16 pounds just by taking the drug within a matter of weeks.
Why is there so much pushback?
One big criticism about these drugs as a solution is the position that they do not resolve the underlying issues attributable to obesity and bad health. Poor diets account for one in five deaths globally, more than any other risk including smoking, a Lancet study found in 2019. A lot of that has to do with people eating too much sodium and not enough whole grains and fruits, the research concluded. Americans are also eating too much processed meat and not enough of the healthy fats in seafood, nuts and seeds — trends associated with heart disease, stroke and type 2 diabetes deaths.
Another critique stems from the focus that the media put upon weight loss. Although weight can be an indicator of overall health, it definitely is not the same thing. Neglecting the quality of diets could result in malnutrition, cardiovascular disease, cancer, and other chronic conditions.
There is also buzz about the impact sudden weight loss can have on facial skin:
What are the supporters saying?
As much as there is something intuitively odd about a diabetes drug being prescribed for obesity, as this Dr. Nisha Patel explains for the Obesity Action Committee, Type 2 diabetes and obesity are actually related conditions:
Therefore, any “off-label” or repurposed use, according to some doctors, should really not be that offensive.
There are also increasing reports of success in fighting various addictions by suppressing urges, whether it be related to alcohol, nicotine, gambling, or shopping. An article going viral in the Atlantic asks, Did Scientists Accidentally Invent an Anti-addiction Drug?
Doctors that are prescribing the drugs are not limited to the internal medicine kind you would expect. Psychiatrists are prescribing the drugs as a form of restitution for patients that have endured weight gain from various anti-depressants, particularly SSRIs. “If I caused it, I prescribe it, is basically my mandate,” says a consultant to DAOFitLife, medical doctor and psychiatrist, Dr. Jason Rosen, If you want to read more about SSRI medication and dealing with the weight gain fall-out, definitely check out my article here:
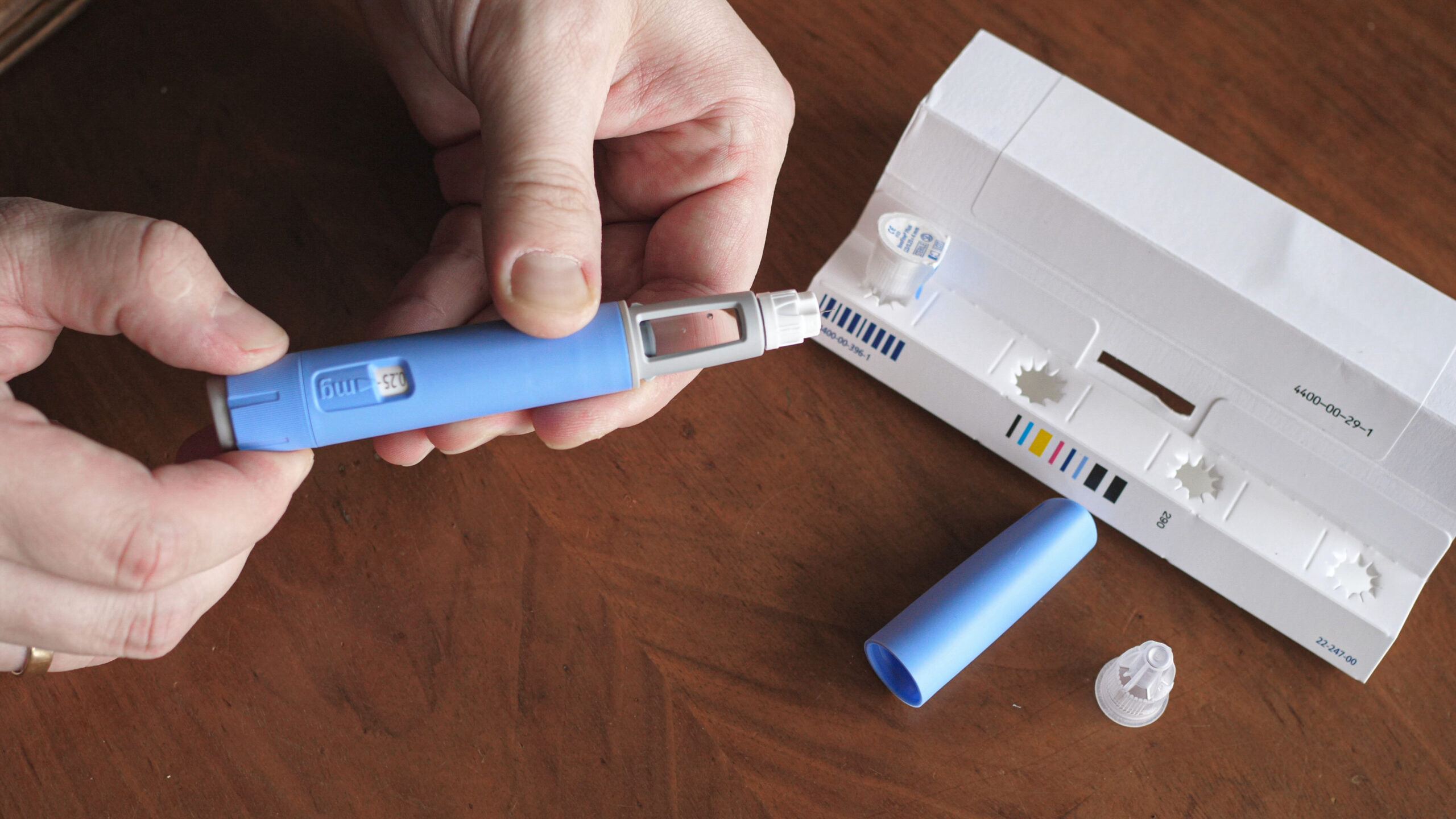
How are the drugs taken?
Injectable semaglutide weight loss drugs are typically administered subcutaneously (under the skin) using a pre-filled pen device. The pen contains a single dose of the medication and is designed for easy self-administration.
The standard dosing regimen for semaglutide weight loss treatment is once a week. The initial dosage of semaglutide for weight loss is typically lower and gradually increased over a few weeks to minimize potential side effects. Regular follow-up appointments with a healthcare professional are recommended to monitor progress, discuss any concerns or side effects, and make necessary adjustments to the treatment plan if required.

How much do they cost? Are they insured?
When prescribed off-label, insurance will usually deny coverage for these drugs. Even the FDA-approved drug for weight loss has spotty insurance coverage, so users can be looking at a monthly cost of at least 1000 dollars, or more, with an average cost of about 1200 dollars per month.
What are the possible side effects?
Known side effects include vomiting, headaches, nausea, digestive issues, increased heart rate, and dizziness. More serious risks and/or side effects include acute pancreatitis, acute gallbladder issues, kidney injury, and thyroid cancers.
Moreover, due to the newness of this drug, there are unknown side effects in the long term.
This video has a great explanation of the possible side effects:
Will you gain the weight back when you stop using it ?
In the same tweet, Andy Cohen also wondered, “What happens when people stop taking [it]???” Good question, Andy.
It’s a complicated answer with spotty data. Even while still on the drug, plateauing is a possibility. According to this article in the US News and World Report, weight loss from the medication generally plateaus around 3-6 months. Once the medication’s effect on weight loss wears off, it can be extremely easy to gain weight back again. In order to avoid weight regain, the person must follow a very strict diet and lifestyle change.
Further, a study published in the Journal of the American Medical Association, that found that people who took injectable semaglutide regained two-thirds of the weight they had lost when they went off the drug. This is known as a “rebound” effect and can happen after any dramatic fast weight loss process.Once your body gets used to consuming so few calories, a form of metabolic adaptation occurs where your body is used to the fewer calories you are consuming. Once your appetite returns to normal and calorie intake increases, however, that will naturally cause weight gain as your body has now “adapted” to eating less. Contestants of the TV show “The Biggest Loser” had experienced a decrease in resting metabolic rate that still persisted 6 years after the competition had ended.

Is there an OTC version?
Sort of…but not really. An over the counter herb is being marketed as “nature’s Ozempic,” called berberine, that is said to reduce blood sugar in a way that mimics the effects of semaglutide. However, these claims are met with intense skepticism, especially since semaglutide does not exist in nature.
Can you reduce your appetite without taking anything at all?
Interestingly enough, there is apparently behavior you can follow to mimic the “slow stomach emptying” effects. By eating and chewing more SLOWLY, your brain will receive a signal of fullness as hormones are released through the gut. In a 2019 study, clinical participants also reported a greater reduction in appetite from eating more slowly.

If you are not diabetic but want to lose weight, should you consider these drugs?
Like with any prescription drug, this is only for you and your doctor to decide. Note that the prescription guidelines for these drugs as a weight loss tool are fairly strict. If you’re prescribed it for weight loss, it’s after a consultation with a medical professional who deems your weight such a risk factor, it’s vital for you to lose weight to stay alive. “There are strict guidelines for its use and clinical criteria need to be met before it can be prescribe,” as one doctor explains to Marie Claire UK.
According to Healthline Magazine, experts share that people who are not diabetic or obese should not use Wegovy or Ozempic for any reason, including to lose small amounts of weight. Nevertheless, the New Yorker recently did an expose where the writer was easily able to get a telehealth appointment and access to a prescription for compounded semaglutide.
To even further complicate matters, lawsuits against medical spas are happening because these entities are selling their own custom-made versions of the semaglutide, as reported by the Wall Street Journal.

Diet culture v. an epidemic
What the current craze really commands we think about is what happened to the “curvy is in” culture? When did “thin is in” suddenly make a comeback? I definitely don’t think the drugs or their manufacturers are to blame. This is a question of supply and demand. And It’s not just the US – apparently the drugs are taking China by storm.
The current zeitgeist around “thin is in” catapults me back to growing up in the 90s, when clavicles were badges of beauty and a sunken-cheeked Kate Moss glared at us from magazine covers. The supermodel is credited with the quote, “Nothing tastes as good as skinny feels.” This was echoed by our mothers warning us, “a moment on the lips…a lifetime on the hips!!” We were told by fitness magazines to drink a big glass of water if we were hungry, because we were really thirsty. There were actual stores that only carried up to a size 5.
On the other hand, according to Forbes Magazine, 4 million people die from obesity-related causes per year. The worldwide rate has doubled since 1980 alone. So what’s the right balance here?
There are no black or white answers, but there will be updates that I will definitely share!
More reading
- Life after food (the CUT)
- Diabetes Drug Ozempic Trends On TikTok As Weight-Loss Drug (YouTube)
- Wegovy v. Ozempic (UC Health)
- Weighing the Facts: The Tough Truth About Weight Loss (Michigan medicine)
- A diabetes drug is going viral for its supposed weight loss benefits—but there’s a seriously dark problem here (Marie Claire UK)